The Ultimate Guide to Understanding and Treating Finger and Toenail Fungus

The following resource represents a culmination of The Global Nail Fungus Organization's efforts over the last 10 years to create the very best resources on finger and toenail fungus. Coming in at over 20,000 words this page features deep and well-researched information from the best sources across the medical world. We view this comprehensive guide as our flag-ship resource and will continue to update it on a consistent basis to ensure it remains current, accurate, and the best resource on the internet for understanding and treating finger and toenail fungus.

I. Nail Fungus Overview
What is a Nail Fungal Infection?
Nail fungus infection, also known as onychomycosis or Tinea Unguium, is a very common condition that is characterized by changes in the nail’s color and texture. The signs of a fungal infection start with the development of black or brown spots and white or yellow streaks under the toenail or fingernail. As the fungal infection progresses, the discoloration would spread, and the infected nails may change to yellow, green, white, or brown. Infected nails may also appear thickened and have crumbled edges. Although this condition is generally not painful, in rare and severe cases, pain and discomfort has been reported by affected individuals. Detachment of the nail from the nail bed may also occur.

Nail fungus is commonly caused by microscopic fungi (called dermatophytes) that enter your toenails, fingernails, and even the skin under your nail (called the nail bed) through small cuts and cracks in the nail or on the surrounding skin. Nail fungus infection happens when there is an overgrowth of these dermatophytes.

There are several treatment options available for nail fungal infection. Choosing which one to undergo depends on the severity of the case. For mild to moderate cases of onychomycosis, over-the-counter and prescription-only oral medications and topical solutions are available. For severe cases, non-surgical procedures (like laser treatments) and surgical procedures (like avulsion) can be done to the infected nail(s). However, because these fungi are often stubborn to cure, a recurrence of the nail fungus infection is still highly possible even after treatment. Precautionary steps such as proper hygiene and regular application of a recommended topical solution is advised to avoid an onychomycosis relapse.
When diagnosing a fungal nail infection, a medical specialist (such as a dermatologist or a podiatrist) would have to rule out other relevant conditions because of some similarities in their symptoms. The next section discusses these other conditions often confused or mistaken with onychomycosis.
Differentiating Nail Fungus From Other Nail Abnormalities
A nail fungus infection is also often associated with nail injury, psoriasis, and melanoma due to some similarities in their symptoms. The following detail conditions which can be confused with symptoms of nail fungus but are NOT NAIL FUNGUS:
Nail Injury
Psoriasis
Skin Cancer/Melanoma
These three conditions typically bear a resemblance to nail fungal infections, but one of the most identifiable difference of onychomycosis from these other nail conditions is the nail’s emission of a foul odor. This can be a symptom more connected to the presence of a nail fungus condition.
Nail Fungus Statistics
- USA and Canada
- Europe
- ASIA
According to an analysis from NC State University, there are an estimated 2%-18% of people who are affected by nail fungal infections worldwide. Another study reported that onychomycosis has an international prevalence range of 3-26% worldwide.
A research report also demonstrated that toenail onychomycosis is the most difficult fungal infection to cure. According to the results they’ve gathered, onychomycosis prevalence rates in different parts of the world are the following:
- 14% in North America
- 23% across Europe
- 20% in East Asia
Pathogenesis: Stages of Nail Fungus Development

Anatomy of the Nail
The nail is an important part of the integumentary organ system that protects and covers the tips of human toes and fingers. It is made of a tough protective protein called keratin.
Nails consist of the matrix, lunula, nail bed, nail sinus, nail plate, free margin, hyponychium, onychodermal band, eponychium, perionyx, cuticle, lateral margin, nail groove, nail wall, and paronychium.
Each of these nail parts are explained in detail within the dropdown box below:
Parts of the Nail Explained
Nail Fungus Development



Nail fungus typically develops when there is an overgrowth of dermatophytes (a kind of pathogenic fungi that can grow on skin areas and cause skin diseases) in, on, or under the nail. In a few cases, it can also be caused by non-dermatophytic molds and Candida yeasts.
Dermatophytes, mold spores, and yeasts can penetrate the nail through small cuts in the skin surrounding your nail, a crack in your nail, or any separation between your nails, fingers, or toes. Under warm and moist conditions, these microorganisms can thrive and rapidly grow. They will feed on the keratinized tissue of the nail in order to nourish themselves. Aside from that, they will also produce byproducts that are harmful for the nail structure which causes the infection, the changes, and the degradation of the nail. As the fungal colony grows, the rate in which the nail host becomes damaged also increases. Meanwhile, as the body tries to repair the damage that’s happening on the nail, it will increase its production of keratin on the affected area. This in turn is what makes the nail thickened. Eventually, if left untreated and the growth of the fungal colony continues, the nail may become too weak to support itself and can lead to it falling of. In some severe cases, the infection may also cause pain.
A more detailed discussion of the causes of nail fungal infection is discussed in the next section.

II. Nail Fungus Causes
An overgrowth of pathogens in your nail area causes nail fungus. As fungus (a kind of pathogen) thrive in warm and moist environments, the feet are more prone to getting in contact with fungus (i.e. by wearing sweaty socks in tight shoes for a long time or by walking barefoot on wet and humid places like the public sauna, spas, community pools, etc.). The toes also have less blood flow than the fingers, which makes it harder for the body’s immune system to detect and block the infection. Thus, toenail fungal infection is more common, and it typically occurs in about 10% - 20% of the adult population. However, the occurrence of fingernail fungal infection is still possible if fingers are constantly kept wet or damp and if they are exposed to dermatophytes.
Pathogens typically infect a nail by penetrating it through small cuts in the skin surrounding your nail, a crack in your nail, or any separation between your nails and fingers or toes.
If left untreated, your the condition may become more severe. Fungal infections are also very contagious and can spread to your other nails and skin.
Pathogens Causing Nail Fungus
One or a combination of the three types of pathogens can cause nail fungal infections. These pathogens are dermatophytes, candida, and non-dermatophytes. Dermatophytes are the most common cause of onychomycosis. Candida and molds cause 8% and 2% of fungal nail infections respectively.
The skin’s outer layer typically has the ability to discourage microorganism’s colonization. Shedding of epidermal cells also helps in avoiding microbes’ growth. However, due to trauma, maceration, and irritation, the skin’s protection mechanisms may fail. This results to susceptibility to infections.
Dermatophytes
Dermatophytes are among the types of fungi that invade dead keratin tissues. This is the reason why they are the most common cause of infections in the nails, hair, and skin. Dermatophytes has no ability to penetrate living tissues.
Trichophyton rubrum is the most common type of dermatophyte that causes athlete’s foot and onychomycosis. It accounts for about 70% of the total onychomycosis cases.
rubrum originated in Southeast Asia, Indonesia, Northern Australia, and West Africa, which later spread to the United States of America and Europe in the late 19th and early 20th centuries. Dermatophytes can be spread through direct skin-to-skin contact with infected people, animals, soil, and objects.
Candida
Candida is a type of yeast that also causes fungal infections. Yeasts are normally present on the human body and are usually harmless. However, yeast overgrowth — caused by illness, birth control or antibiotic pill intake, and immune system problems — may lead to a yeast infection.
Candida species may also invade previously damaged nails from trauma or infection. It more commonly affects the hands and typically occurs in individuals who constantly have damp hands.
Non-Dermatophytes/Molds
Non-dermatophytic molds (NDMs) are among the types of fungi that grow in soil, skin, and nails. These do not typically spread through person-to-person contamination. NDMs typically occur together with dermatophyte fungal infections. Conclusions from studies suggest that these are largely considered as contaminating organisms in dermatophyte onychomycosis.
Another study suggests that nails should be tested for non-dermatophyte molds if dermatophyte infection treatments are not effective. Even though an infection has no dermatophyte present, the possibility of an NDM infection should not be omitted. There has been a reported rise of onychomycosis caused by non-dermatophyte molds in Gyeongju Korea (2012) and South-East Rajasthan (2015).
Nail Fungus Risk Factors
There are different modifiable and non-modifiable factors that affect your susceptibility to fungal infections. This includes your overall health, your environment’s humidity and heat levels, and the condition of the nail(s) infected, among others.
Non-Modifiable Factors
Non-modifiable factors that increase your risk of nail fungus infection development are age, gender, and existing condition. Below are some key points that further discuss these factors:
Age
Studies from different countries show that individuals older than 60, are prone to nail fungal infections. As we age, we experience a decrease in our blood’s circulation around our hands and feet. In order to deliver immune fighting bodies which detect and combat invaders, such as fungi, blood flow should be normal. This is why decreased blood flow in older adults is a problem that increases their susceptibility to fungal infections such as onychomycosis.
Gender
Males are reported to be up to three times more likely to acquire nail fungal infections than women, especially those who have a family history of onychomycosis.
Existing Health Condition
Having a nail injury, skin condition like psoriasis, as well as other diseases such as diabetes, peripheral arterial disease, HIV, and cancer increases the susceptibility to fungal nail infections. This is due to spreading of infection, poor circulation problems and a weakened immune system brought by these conditions and some of their medications such as steroids and chemotherapy.
Existing Health Conditions Details
Modifiable Factors
There are numerous factors that you can control and avoid. You must keep in mind that you can develop nail fungal infections through the following:
Walking Barefoot in Public Places
Walking barefoot in moist and warm areas like public showers, community pools and locker rooms, and spas increases your risk for nail fungal infections. These are areas where you can be exposed to fungi from other infected people.
Working Conditions
As discussed earlier, fungi grow and survive in high moisture environments. Working in hot and moist environments, especially with wet hands or feet, puts yourself at risk for fungi reproduction and infection.
Wearing Heavy Footwear
Wearing heavy footwear that hinder proper ventilation throughout the feet makes them more damp with sweat. Sweaty socks as a result of the lack of airflow on heavy footwear is one of the top causes of fungi growth and multiplication that eventually leads to toenail infection.
Working with abrasive chemicals
Exposing your hands to abrasive chemicals may cause damage to the protective skin at the base of your nail, which makes it more vulnerable to fungal penetration.
Sharing nail care tools
Nail fungus is highly contagious. You can have onychomycosis from someone with infected nails. Sharing a towel or nail care tools with an infected person increases the possibility of being infected by a fungus.
Injuring your nails
If you have injured nails, you are more vulnerable to fungi infection due to easier penetration and infection from cuts, tears, or thin protective layers of your nails.
Going to unhygienic/ unregulated nail salons/spas
As mentioned above, sharing nail care tools with fungi-infected individuals should be avoided. You should ensure that the nail salons, parlors, and spas you are visiting use disinfected equipment and new towels as nail fungi can be transmitted through these tools.
Living with someone who has nail fungus
Fungi is contagious and can be picked up through skin-to-skin contact. Living with a fungi-infected individual can put you at risk, especially if you are sharing items with that person.

III. Nail Fungus Signs and Symptoms
Nail fungus may affect a nail fully or partially, and may spread to other fingernails and toenails. In more severe cases, it may also affect the skin around your nails.
Early Signs and Symptoms
As the condition is generally not painful, paying attention to any change in appearance and texture on your nail may help you detect the problem early on.
Nail discoloration
Changes in the nail’s color might be the first sign of the presence of fungus on your nail.
White, yellow, or dark-colored spots may appear on or under your nail (proximal onychomycosis); or you might notice flaking white areas on the nail’s surface. In other cases, white, yellow, or brown streaks or lines may occur on the nail (lateral onychomycosis) or the whole nail turns white, yellow, brown, green, or black.
Change in nail’s texture/shape
Changes in the nail’s texture may include pitting of the nails, characterized by depressions on the nail’s surface and scaling under the nail (subungual hyperkeratosis).
The nail may curve in on the sides, take on an unusual shape, and become thickened at the center — making it difficult to trim.
Brittleness
The corner or tip of the nail may crumble (distal onychomycosis), making pieces break off easily.



Severe Signs and Symptoms
As the infection progresses, other symptoms may start manifesting, such as:
Unpleasant odor:
a foul odor emanates from the affected nail.
Chipping off:
the tips of the nail might break or chip off, causing jagged edges. Upper layers of the nail might start peeling off.
Loss of nails:
in more severe cases, a condition called onycholysis occurs, wherein the infected nail disengages from the nail bed and leads to the partial or total loss of the nail.
Decayed / diseased nails:
the infection promotes the decay of the nail.


IV. Nail Fungus Classification
Distal Subungual Onychomycosis (DSO)
This is the most common type of fungal nail infection, and it is usually caused by trichophyton rubrum, a dermatophytic fungus. DSO starts on the end of the nail bed and the underside of the nail plate. It may be difficult to treat this completely, and can become a lifelong condition.
In some instances, DSO may be caused by wearing closed shoes that fit too tightly for prolonged periods of time. Once the infection starts, wearing closed shoes might become uncomfortable and make the infection worse.
The progression of DSO includes:
- The nail often turns yellow or white partially or completely
- Pieces of debris made up of skin and nail fragments begin to build up under the nail
- The nail may eventually crumble, split and disengage from the nail bed
- Thickened nail
White Superficial Onychomycosis (WSO)
This condition makes up 10 percent of nail fungal infection cases and is most commonly caused by Trichophyton mentagrophyte, another type of dermatophytic fungus.
It occurs on the uppermost layer of the nail plate and usually affects the toenails. WSO can be treated quickly.
The signs associated with WSO include:
- Opaque white spots or ‘islands’ on the nail’s surface
- The whole nail might eventually turn white, soft and crumbly
Proximal Subungual Onychomycosis (PSO)
Proximal Subungual Onychomycosis is another type of nail fungus which is also caused by dermatophytes, usually trichophyton rubrum in particular. PSO occurs on the proximal nail fold (skin at the nail fold) and may penetrate the nail plate.
This condition may affect the fingernails and toenails in equal frequency. It commonly occurs in people with compromised immune systems and is considered one of the symptoms of human immunodeficiency virus (HIV) infection. It may also develop due to nail trauma.
PSO may appear in the following ways:
- Thickened skin at the nail fold, which may cause the skin to separate from the nail
- The nail color may become opaque white
Candida Infections of the Nail
Otherwise known as yeast infection of the nail, this condition is less common and may also affect the skin around the nail. It occurs more frequently on the fingernails than the toenails, and may invade nails weakened by previous infection or trauma. People who habitually immerse their hands in water are at high risk of developing this type of nail fungus infection.
Candida onychomycosis is usually characterized by:
- Separation of the nail from the nail bed (onycholysis)
- Discoloration of the nail- color might turn to white, green or brown
- Abnormality of the nail shape
- Thickened nail
- The skin around the nail (nail fold) may become swollen and tender
- The site of the infection may become painful
Total Dystrophic Onychomycosis
This condition refers to the complete destruction of the nail plate and may be the end result of any of the four types of nail fungus infection above.
Nail Fungus Gallery





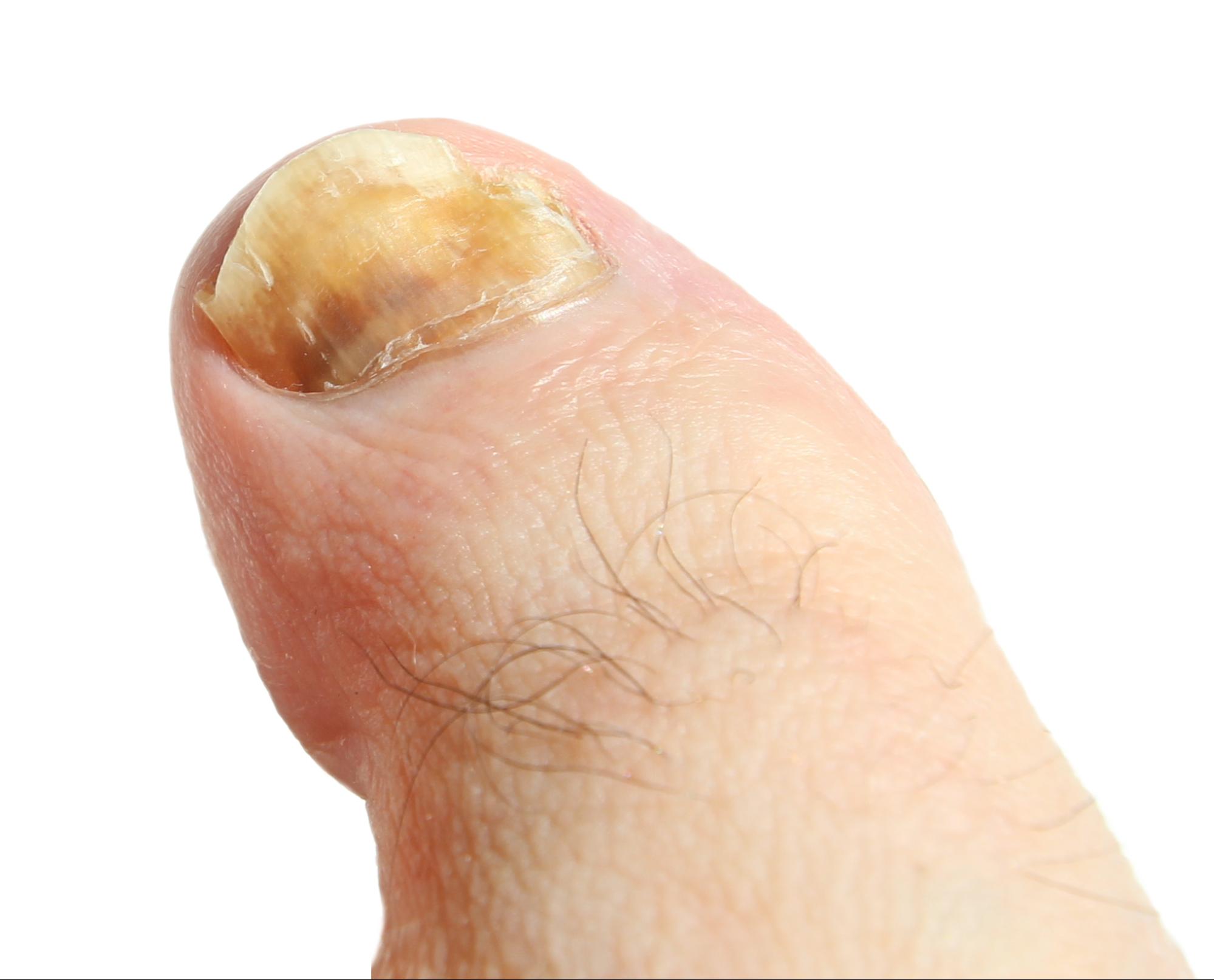
V. Test and Diagnosis of Nail Fungus
Nail Clinical Examination
In order to ensure that your nail abnormalities are caused by fungal infections and not by other conditions that share symptoms with onychomycosis, a doctor’s diagnosis is required. This is vital in making sure that the recommended treatment will be effective for that specific case of onychomycosis.
Before giving their diagnosis, doctors conduct careful physical examination of your infected nails and surrounding skin, as well as an interview about the symptoms you’re experiencing and your medical history. These are beneficial in differentiating fungal from non fungal causes of your nail abnormalities.
Common clinical characteristics of onychomycosis-affected nails are white/yellow or orange/brown streaks in the nail plate. However, nonspecific findings include: nail thickening, onycholysis (which is the separation of the nail from its nail bed), and subungual hyperkeratosis (which is the excessive build up of the nail bed and the hyponychium).
Specialists also look for a match of your conditions and the physical characteristics of the five classifications of onychomycosis as discussed in the previous section.
Aside from examining the physical appearance of your nails, predisposing factors for onychomycosis are also considered. These are: older age, immunodeficiency, poor circulation, diabetes, and others which are also further discussed in Section 2. The existence of these factors and characteristics raises the clinical suspicion of onychomycosis.
It should also be noted that before undergoing laboratory tests, these considerations must be acknowledged:
- Nail material should be sent for microscopy if treatment will be given. Even though there is a 30% to 40% false negative rate, positive results should be carefully interpreted as it cannot be automatically considered as an invasive infection.
- Nail sample culturing may take several weeks but should be undertaken to determine the species that cause your nail abnormalities.
- Nail histology is not usually required, except for cases where another cause of nail changes is suspected.
Only about one half of nail dystrophies are caused by fungus, so in order to ensure correct diagnosis, laboratory testing may still be required.
Collecting Nail Specimen
In order to run laboratory tests to confirm diagnosis, samples should be collected from the infected nails. The sample collection process begins with thorough cleansing of the infected nail area and surrounding skin with 70% alcohol to eliminate other contaminants.
Obtaining optimal nail specimens depends on the presumptive diagnosis and site of the infection. The following approaches are recommended:
For Distal Subungual Onychomycosis (DSO)
For Proximal Subungual Onychomycosis
For Candida Onychomycosis
For White Superficial Onychomycosis
Laboratory Test
After collecting infected nail samples and skin scrapings, specimen analysis and antifungal susceptibility tests are conducted. First, the laboratory experts will examine the nail and skin scrapings to identify the type of organism that causes your infection. Below is a thorough discussion of these examinations.
Microscopy, staining, and culturing procedures may take up to six weeks before results can be received. Another generic test called the polymerase chain reaction (PCR), a method of detecting dermatophytes, delivers results within hours. The main approaches of laboratory confirmation of the diagnosis are the following:
- Potassium hydroxide smear
- Culture
- Histology
These comprises of the microscopic examination and culture of the obtained nail and skin debris. In identifying nondermatophyte molds, collecting several samples may be required. Results from these tests will strengthen the diagnosis and are also vital to formulating the proper treatment plan.
Specimen Analysis
Antifungal Susceptibility Testing
VI. Treatment of Finger and Toenail Fungus
Treatment Selection
As mentioned in an earlier section, a dermatologist (skin doctor) or a podiatrist (foot doctor) will start with a physical examination of the infected toenail or fingernail. Debris under the nail, a portion of the nail, or affected skin tissues may be collected for further microscopic testing and culture. The test will be able to determine the cause of the infection: fungus, yeast, or molds.
- 2. Fungus Identification
- 3. Patient Considerations
Classifying Severity of Nail Fungus
Your doctor will determine the severity of the condition based on the symptoms present.
As discussed in the “Nails Fungus Signs and Symptoms” section, signs such as nail discoloration and change in the nail’s shape and texture may indicate that the infection is on its early stages and may be considered as mild.
Other symptoms, such as an unpleasant odor, chipping off of the nail, loss of nails, and a decayed appearance of the nail, may signal that the infection has progressed to moderate or severe level.
An infection that affects more than 50% of the nail is considered a severe form of nail fungus infection.
How to Know What Type of Treatment Would Work Best for You?
In the recent years, there has been a more optimistic outlook on the treatment outcome of patients with nail fungus due to the introduction of promising new options, such as itraconazole, terbinafine and fluconazole. A personalized treatment plan that factors in a patient’s profile, symptoms, infection type, drug toxicities and interactions, is shown to result to improved success rates.
Below, we explore more details about the available treatment options.
Types of Treatment
Over The Counter (OTC) Topical Treatments

Over the counter / non-prescription topical solutions may be used for the treatment of mild nail fungus infection.
As these therapies usually contain natural ingredients, they are safe to use with minimal contraindications, so you can use two or more remedies together. They are relatively inexpensive but may take several months to fully take effect.
These topical remedies penetrate deeper into the layers of the nail when the nail is clean, trimmed and thinned. To clean the nail, soak it daily in a baking soda, hydrogen peroxide and water mixture.
These over the counter treatments have not been comprehensively evaluated in clinical studies. The limited trials done involved only a small number of patients.
Common ingredients used in non-prescription topical agents include:
Undecylenic acid
Tea tree oil (melaleuca alternifolia)
Sunflower seed oil (ozonized)
Snakeroot extract (ageratina pichinchensis)
Coconut oil
Lavender oil
Garlic
Tolnaftate
Some individuals opt for over the counter topical creams and prepared solutions, as they are more convenient to use. These well-known topical solutions already contain one or a combination of the active ingredients above:
EmoniNail
Funginix (Fungisil)
ZetaClear
Naturasil (formerly Dermisil)
Pedifix Fungasoap (Tea Tree Ultimates Fungasoap)
OPI Fungus Fix
Omega Labs Fungus Treatment
Fungi-Nail Brand
Excilor
RX/Prescription Medication
Topical Rx Antifungal Medications
Prescription topical solutions are also available for the treatment of nail fungus. Treatment with topical agents alone are generally shown to be insufficient, due to lack of penetration through the nail bed.
Topical agents have few contraindications and drug interaction. However, they may result to adverse effects, such as redness, stinging and itching on the application site.
Nail debridement and trimming may be done beforehand by your doctor to help the agent penetrate the nail more efficiently. A lotion containing urea as the active ingredient can also work in thinning the nail. Nail avulsion (a surgical procedure involving the removal of the nail plate from its attachments and the nail bed) combined with topical therapy has yielded more positive results. However, this method is painful and recovery from the surgery might take a long time.
A combination of prescription oral medication and topical antifungal preparations may be recommended for moderate to severe cases of nail fungus infection.
Topical therapy may be continued after the course of oral prescription medicine to help prevent the recurrence of the infection.
The most widely-used prescription topical medications currently available in the market are:
Tavaborole (Brand Name: Kerydin)
Efinaconazole (Brand Name: Jublia)
Ciclopirox (Brand name: Penlac)
Oral Rx Antifungal Medications
Oral antifungal agents may be used for the treatment of moderate to severe nail fungus infection. Oral medications under the azoles and allylamines drug classes are most commonly prescribed.
Azole antifungals work by inhibiting the cytochrome P450 dependent enzyme lanosterol 14-alpha-demethylase. This action depletes ergosterol, which leads to the cell death of fungal cells. Itraconazole and fluconazole belong to the azole family.
Allylamine antifungal agents also hinder the synthesis of ergosterol, by inhibiting the enzyme squalene epoxidase. Terbinafine is under the allylamine medication class.
These drugs are typically taken for a period of six to twelve weeks. However, you need to wait for the healthy nail to grow back completely before you will see the end result.
Clinical studies show that the combination of oral and topical antifungal therapies is more effective, compared to treatments using a single approach. (See above for data on lower cure rates of terbinafine solo treatment versus terbinafine-ciclopirox combination)
Possible adverse effects of these oral antifungal medications include headaches, gastrointestinal problems, and skin rashes. Serious medical conditions associated with the use of these drugs are Stevens-Johnson syndrome (a life-threatening skin disease), Long QT syndrome (a heart rhythm condition), ventricular dysfunction and liver damage. Patients with renal, heart or liver issues are discouraged from taking oral antifungal agents. Blood tests to check the liver function are usually done before beginning oral therapy and after every 6 weeks of treatment.
More detailed information on the uses, clinical studies results, contraindications, and side effects of the top oral antifungal agents for the treatment of nail fungus infection are given below:
Griseofulvin (Brand names: Fulcin, Grisovin, Grisactin, Gris-PEG)
Terbinafine (Brand name: Lamisil)
Itraconazole (Brand name: Sporonox)
Fluconazole (Brand name: Diflucan)
Nail Removal
Though rarely necessary, your podiatrist, dermatologist or general surgeon may suggest nail avulsion or removal for severe or recurrent nail fungus infection — especially when a large portion of the nail is diseased, the nail is extensively thickened or the condition is painful. Nail removal is an outpatient procedure done in your doctor’s clinic or office.
Nail removal makes it possible to apply topical antifungal solutions directly to your nail bed, improving the absorption of the agent and increasing the chance of curing severe nail infections.
The procedure must be accompanied by topical or oral antifungal therapy to kill the fungi and other organisms. Otherwise, the infection can affect the new nail that grows. It may take 6 months for the new fingernail and 12 to 18 months for the new toenail to grow back.
Nail avulsion can be done chemically or surgically; it can be partial (only damaged portion of the nail) or total (whole nail), depending on the extent of the infection.
After the nail is removed, it is important to keep the area clean as the open wound has a big chance of becoming infected. Follow your doctor’s step-by-step care guide to ensure successful results. A highly absorbent dressing and an elastoplast or a paper tape are typically used to cover the operated area and to keep the dressing in place. The dressing may be removed after 24 hours and it is advised to soak the area in warm water or saline solution twice a day. A povidone-iodine solution may also be applied to help quicken the healing process.
The operated limb must be frequently elevated to minimize pain and swelling and it is best to keep it well-rested for at least 2 weeks. Handling the nail matrix and nail folds gently is crucial to avoid complications after the procedure.
In some cases, the patient may opt to permanently prevent a new nail from growing back. The doctor will then surgically, chemically or electrically destroy the nail matrix (matricectomy) so that the nail plate cannot be regenerated.
- Surgical nail avulsion
This non-surgical technique is generally painless and usually involves partial nail removal.
The steps for chemical nail removal include:
- A cloth adhesive tape is placed on the skin around the nail that is to be removed. This is to prevent the solution from getting into and irritating the soft skin tissue.
- In cases when there is gross thickening of the nail, superficial nail abrasion may be done first to improve the solution’s penetration into the nail.
- A 40% to 50% urea ointment/solution (with 5% white beeswax or paraffin, 20% anhydrous lanolin and 35% white petrolatum) is applied directly on the nail surface and covered with plastic and hypoallergenic tape. The nail and dressing must always be kept dry as water may counteract the efficacy of the solution.
- The urea ointment/solution softens the nail within the following one week to 10 days.
- After the nail has softened, it will be removed either by detaching the nail plate from the nail bed (total removal) or by trimming out only the diseased portion of the nail (partial removal).
- The area must always be kept clean. You may cover it with a nonstick bandage. It would take around 2 weeks to heal.
- Continue with your oral or topical nail fungus medications, as advised by your doctor.
Other formulations that showed positive results in softening the nail are: 20% urea and 10% salicylic acid ointment; and 1% fluconazole and 20% urea mixed with ethanol and water (applied once daily in the evening).
Chemical nail avulsion is the preferred nail removal method for patients with diabetes, heart problems or immunosuppression.
The advantages of this method compared to surgical nail avulsion include: minimal pain during and after the procedure (no need for anesthesia), low infection and hemorrhage risk, and shorter downtime.
Disadvantages include: length of application duration (one to two weeks), and possible irritation due to the acidity of the urea solution.
Laser Treatment
Laser therapy is a relatively new option for the treatment of stubborn nail fungus infection.
Some experts see laser as the answer to the challenges of penetrating the hard surface of the nail plate using topical antifungal agents, the potential serious adverse effects of oral antifungal therapy, as well as the pain and risks associated with nail removal. (example: http://www.bvfootclinic.com/laser-toenail-fungus/)
Lasers utilize light energy with the right strength and wavelength to target infected tissues. High doses of light energy can penetrate into the specified area and destroy the fungus and other harmful organisms.
Laser treatment do not minimize the risk of nail fungus infection recurrence, and it is recommended that nail care techniques are implemented afterwards.
Initial research pointed to the effectiveness of this method in treating nail fungus infection, but there is still inadequate evidence to fully support laser therapy as a routine treatment for the condition.
The downside of laser treatment is the high cost associated with it, which is typically not covered by health insurance- as it is considered an aesthetic/cosmetic procedure.
The current top FDA-cleared brands of laser machines for the treatment of nail fungus infection are:
- Noveon laser
- Erchonia Lunula
- Hyperion HyperBlue
- Cutera Genesis Plus
Pinpointe FootLaser
The first FDA cleared laser for the temporary increase of clear, healthy nail in patients with nail fungus infection.
It works by emitting laser light that passes through the nail without causing damage to the nail unit or the surrounding skin. Results are not instantaneous though, as it takes time for the affected nail to grow out.
Clinical studies show that with only a single session, more than 70% of patients reported sustained improvement in nail appearance. This outpatient procedure takes around 30 minutes to complete, is virtually painless (some patients may experience a warming or a slight pinprick sensation) and requires no recovery period.
A Pinpointe Footlaser procedure typically costs around $1,000.
Home Remedies
Without treatment, nail fungus infection may persist indefinitely. For individuals who want to treat their condition without the use of harsh chemicals and ingredients that may lead to adverse side effects, there are several home remedies that might do the trick.
These options might work best on mild nail fungus infection or one that is on its early stages. Home remedies are rarely studied in clinical trials, so scientific research to measure their efficacy are usually not available.
As these home remedies are applied topically, it is always best to trim your fingernails or toenails as close to the nail bed as possible to provide easier access and penetration to the source of the infection
These natural treatment options may have been passed down across several generations, through word of mouth. Some people swear by these home remedies for the treatment of nail fungus infection:
Vicks VapoRub
Bleach
Vinegar
Mouthwash
Hydrogen Peroxide
VII. Complications of Nail Fungus if Left Untreated
Compared to other acute and chronic medical conditions, nail fungus infection might not seem like a highly threatening or dangerous disease. Since the infection is not particularly painful, affected individuals might consider it as a purely cosmetic concern and delay seeking advice from their health providers.
However, the longer you wait before treating your condition, the harder it will be to heal successfully. Ignoring a nail fungus infection can lead to serious consequences as the fungus progresses and may cause negative symptoms beyond the aesthetics:
Deformed nails/ Destruction of nails
As the infection grows from the tip towards the cuticle, the nail becomes thickened, discolored, brittle, and eventually appears deformed or misshapen. When this happens, it might lead to discomfort and pain when walking and putting on closed shoes.
Onycholysis– a condition characterized by the separation of the nail plate from the nail bed can also occur. The loose portion or the entire nail may then either fall off on its own or will have to be removed in an avulsion procedure (discussed in detail in the Treatments section). This might lead to the permanent loss of the nail or in more severe cases, several toenails or fingernails.
Spread of infection to other nails
Fungal infections are highly contagious and can easily spread to the skin surrounding the affected nail and to the other nails as well. The skin might become inflamed, itchy, dry, and cracked — and lead to athlete’s foot or tinea pedis. Athlete’s foot causes skin peeling, stinging, blisters, and sores.
Wearing socks and closed shoes for prolonged periods of time can cause the infection to spread quickly, once one of the toenails has been affected.
Spread of fungus around the body
Keeping a harmful organism alive in your nail can cause the infection to migrate to other parts of the body, such as hands, back, and legs. It can also spread to the genitals, inner thighs and buttocks — in a condition called jock itch. Jock itch is characterized by a red, itchy, and usually ring-shaped rash.
One in every two dozen cases of nail fungus infections results to the spread of the infection to other parts of the body. Older people or those with weakened immune systems are especially susceptible to this.
Paronychia
The fungus can create cracks, chips, and openings in the nail and skin, where bacteria can get in and cause a condition called paronychia (whitlow). It usually enters through a break in the skin between the nail fold (cuticle) and the nail plate.
Paronychia can either be acute or chronic: Acute paronychia develops quickly and is usually caused by the Staphylococcus bacteria, while chronic paronychia occurs slowly and is commonly caused by more than one infecting agent, typically Candida yeast and a bacteria.
Symptoms include:
- Red and tender skin around the nail
- Abnormalities in skin shape, color, or texture
- Blisters
- Detachment of the nail plate from the nail bed
Acute paronychia may be treated using home remedies, and oral or topical antibiotics; while chronic paronychia is harder to treat and may require antifungal medication or even nail removal, in very severe cases.
Cellulitis
Bacteria that entered through the cracks and openings in the nail and skin can cause widespread infection in the body. This may lead to cellulitis — a bacterial skin infection that is potentially serious, even deadly, when it spreads into the underlying tissues, lymph nodes, and the bloodstream.
Symptoms of cellulitis include:
- Swollen, inflamed area in the skin that tends to expand or change rapidly
- The area feels warm and tender to the touch
- Fever
- Blisters
- Can spread quickly on different parts of the body
- Usually appears on one side of the body
Cellulitis can have especially serious consequences for people with diabetes, nerve damage, circulation problems, or weakened immune system. It is associated with increased risk of diabetic amputation.
It is strongly recommended that individuals seek immediate medical attention on the first sign of cellulitis, as the infection can cause rapid widespread infection and lead to serious internal damage or even fatality.
VIII: Nail Fungus Prevention
Given the stubborn nature of nail fungus infection, it is best to take a proactive approach to minimize the chance of its occurrence.
As discussed in the above section (Section II: Nail Fungus Cases — Risk Factors), certain people, such as swimmers and those who have diabetes, have a higher likelihood of contracting the infection. People who have suffered from it before are also at high risk of getting it again — as recurrence rate is at 10% to 50%, despite treatment.
It would be wise, especially for these individuals, to take extra precaution to avoid the hassle, costs, and worries of having to deal with nail fungus infection.
A. Food and Supplements
The adage that whatever you put inside your body manifests on the appearance of your hair, skin, and nails is true.
An antifungal diet gets rid of food ingredients that fungal parasites can feed on and in the process, reduces inflammation inside the body. Eliminating sugar and conventional grain products from your diet means starving the parasites and can lead to their death.
These are the inflammatory food you should avoid:
- Sugar is the primary food that fungi crave. These are not just limited to sweets — such as candies, cookies, chocolate bars, doughnuts and baked goods — but also sugar from carbohydrates, dairy, and fruits (see below).
- Conventional grain products — especially those that contain gluten, such as wheat, rye, barley, and oatmeal. White rice and corn are gluten free, but contain a good amount of starch that converts to sugar (glucose).
- Some dairy products such as cow’s milk, cream, and cheese (lactose is also a form of sugar)
- Processed oil products such as corn oil, canola oil, palm oil, vegetable oil, peanut oil, soybean oil, margarine, and shortening
- Processed, cured, and smoked meat and other food products
- Sweet fruits that contain a high amount of fructose must also be limited, including all kinds of dried fruits, banana, grapes, melon, pear, mango, figs, papaya, peach, etc. Fruit juice must be avoided due to its high sugar content
- Certain vegetables — such as potatoes (due to high starch content) and mushrooms (fungal food)
- Alcohol, coffee, fruit juices, carbonated drinks
- Junk food
Pay special attention if you have specific food allergies, as they can cause inflammation and adverse reactions (such as fungal and yeast growth) inside your body. The list of the most allergenic food includes: dairy, eggs, peanuts, and tree nuts (cashew, walnuts), seafood, wheat (gluten), and soy.
Consume more of the following:
- High-fiber food to help rid your stomach of toxins, waste, fat, and cholesterol particles: legumes (split peas, black beans, lentils, lima beans, peas), vegetables (artichokes, broccoli, brussel sprouts, leafy greens), vegetable/green juice, and fruits (berries, avocado)
- Probiotic food to replenish good bacteria and to support your gut health: yogurt (aim for plain yogurt and not those that contain sugar), fermented food such as cultured vegetables (kimchi, sauerkraut), kombucha, and kefir beverages
- High quality protein sourced from hormone-free, grass-fed, pasture-raised, cage-free, and wild-caught chicken, beef, eggs, and fish
- Good fats, such as coconut oil, olive oil, flax seeds, and chia seeds
- Antibacterial and anti-fungal food ingredients, such as garlic, ginger/turmeric, cinnamon, onion, oregano, seaweed, cayenne pepper, etc.
Though not yet backed by medical research, many individuals report good results from taking probiotic supplements. The good, beneficial bacteria provided by probiotics may strengthen the anti-fungal properties of good bacteria that we already have on our skin and help prevent fungal infection from occurring. A weakened immune system is more susceptible to fungal infections, so make sure that you get the right nutrients everyday. You might want to take a good quality multivitamin that contains Vitamin A, Vitamin C, Vitamin D, zinc, and other essential vitamins and minerals.
B. Lifestyle and Environment
Good hygiene is key to preventing nail fungus infection, so it is important to always keep your feet and hands clean and dry.
Here are some other simple practices you can adapt to minimize the risk of contracting nail fungus infection:
- Trim your nails correctly and keep them short: Use sanitized tools and clip your nails straight across. Gently file down thickened areas and sharp edges. Do not trim (or pick at) the skin around your nails.
- Proper cleaning and drying: Using soap and water, wash your hands regularly and your feet at least once a day. Dry thoroughly, including between your fingers and toes.
- Wear clean, moisture-wicking socks: Change your socks everyday, or as often as needed, especially when your feet sweat excessively. Consider copper sole socks, as they have anti-fungal properties.
- Invest in the right footwear: If you need to wear closed shoes, opt for those made with breathable materials, such as canvas or leather. Wear shoes with a wide toe box to avoid cramping your toes, and choose the correct fit: not too small or too big, and make sure your toes are not touching the end of your shoes. Allow your shoes to dry in between uses.
- Sprinkle anti-fungal foot powder: Do this all over your feet before putting on your socks and shoes, to make sure that they remain dry all throughout the day. This can be used on the inside of your shoes as well.
- Do not walk barefoot around warm and moist public areas: This includes communal locker rooms, swimming pool decks, public shower areas, gyms, sauna. Wear flip flop slippers or shower sandals.
- Disinfect regularly: Sanitize your own bathroom floor and shower head, and wash your socks with warm water, detergent, and bleach. Use antibacterial spray on your shoes and expose them to sunlight (not recommended for leather shoes).
- Avoid skin-to-skin contact with people with any kind of skin or nail fungal infection: Fungus can be passed on through skin-to-skin contact, so ask family members and people you interact with regularly to treat their condition ASAP, to avoid the spread of the infection. Do not share footwear and nail tools with other people. Wash your hands thoroughly if you touch infected skin or nails.
- Do not smoke: Smoking increases the chance of getting nail fungus infection.
C. Preventing Reinfection
It is frustrating to have to deal with recurrent cases of fungal nail infection. Apart from the tips given above, you can add the following practices to avoid reinfection:
- Use the medications (oral or topical) completely and correctly as prescribed by your healthcare provider. Be consistent, as the fungus may still be present, even if outward symptoms are no longer visible.
- Watch out for the early signs of the infection: By now, you might already be familiar with the first signs of nail fungus infection (see Nail Fungus Signs and Symptoms section). Visit your doctor immediately once you start noticing nail changes to avoid the infection from progressing further.
- Replace all footwear that have come into contact with the fungus: The harmful organisms may persist inside your shoes, socks, and other footwear for many months, and can easily cause another round of infection. In case you do not want to get rid of your shoes, make sure to sanitize and disinfect them properly. You may also consider investing in a UV sterilizer.
- Soak your hands and feet in an anti-fungal bath regularly: This provides a hostile environment for the fungus and prevents it from growing. A vinegar-water solution (one part vinegar and five parts water) can kill any existing fungus, as the organism cannot survive in an acidic setting. You can also try a saline solution soak (two teaspoons of salt for every pint of warm water).
D. Nail care routines and hygienic practice you can do at home
Bad news for those who love to get their nails done in salons: it can put you at increased risk of getting nail fungus infection. The fungus can spread through the following ways:
- Direct contact between clients
- When the nail technician does not sanitize her hands between servicing different customers
- It can be passed on through the shared nail tools, especially if they are not properly sanitized between uses.
The good news is: it is easy to do your own manicure and pedicure at home. You can avoid the hazards associated with getting your nails done in public salons/spa, and this will help you to save on costs too.
Manicure and Pedicure Procedures
Essential Nail Tools
How to sanitize and clean your nail tools
Recommendations on using nail polish
IX: Frequently Asked Questions on Nail Fungus
Is fingernail fungus as common as toenail fungus?
I’ve been treating my nail fungus for months but haven’t found cure. Is my treatment really working?
Can I still get nail fungus even if I wear nail polishes often?
Can you use topical treatment and nail polish?
X: Best Resources on Nail Fungus
It helps to be armed with the right information in your battle against the stubborn nail fungus infection.
Based on our intensive research, these are the most helpful online resources on the condition: